Kathy’s anterior rehabilitation
Managing a patient’s expecations
Case description
I suppose Aesthetic case studies have been done to death by now, with the general format presenting a series of photos with a happy outcome, in my opinion missing all the valuable parts in between.
I think it’s important to look at the technicalities, the wheres, and the why-fours as to how we achieved an end result that is suitable for a particular patient. It is equally important to talk about the management of a case however big or small. This will, therefore, be more of a reflection point on those cases, on a more emotive level, the learning process for ourselves as technicians but also the patient as we embark on our journey.
In this particular case study, I would also like to discuss the psychological changes that can occur during treatment and how we must adapt our approach. Managing expectation, yet achieving a smile that your patient falls in love with being the ultimate objective.
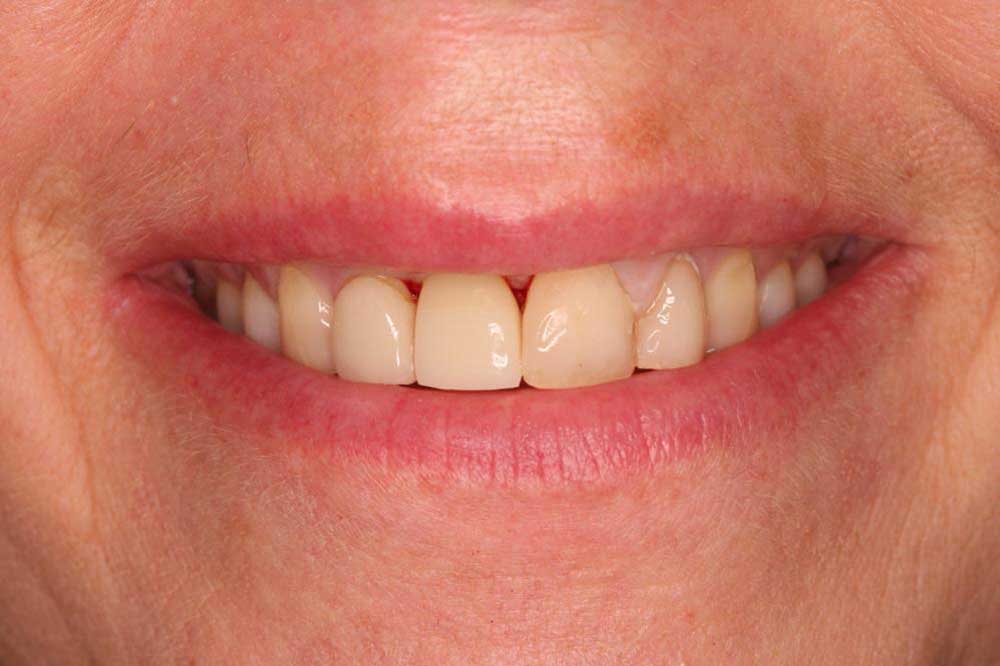
Fig 1- shows how Kathy presented with the inclusion of the immediate load temporary; occasionally as a laboratory we miss the initial photographs especially when they arrive as an emergency.
So, our journey begins
Kathy, who presents as possibly 99% of all other patients do, is someone who has lived with an almost patchwork quilt of previous restorative measures, crowns, veneers and some chairside composite work, for an awfully long time, but now with a root canal on tooth 11 having failed.
Kathy has seen this as an opportunity to address all the other issues that have been niggling her for a number of years with the view that without compromise she would like to be able to smile with confidence again!
As is often the case, patients who have been quietly suffering for long periods of time, not necessarily in terms of pain or discomfort, but suffering in the physiological regard, need 100% focus and attention, as these cases can often misread, with the notion that Patient A or B is just being fussy.
It is crucial that you listen for the signs, as there is a huge difference between someone who is looking to have treatment purely for cosmetic reasons with perfectly vital teeth albeit with some imprecations and someone that presents with clear signs of historical dental work.
This is not age or gender-specific either. This is a huge subject in itself and one I could go over at another time.
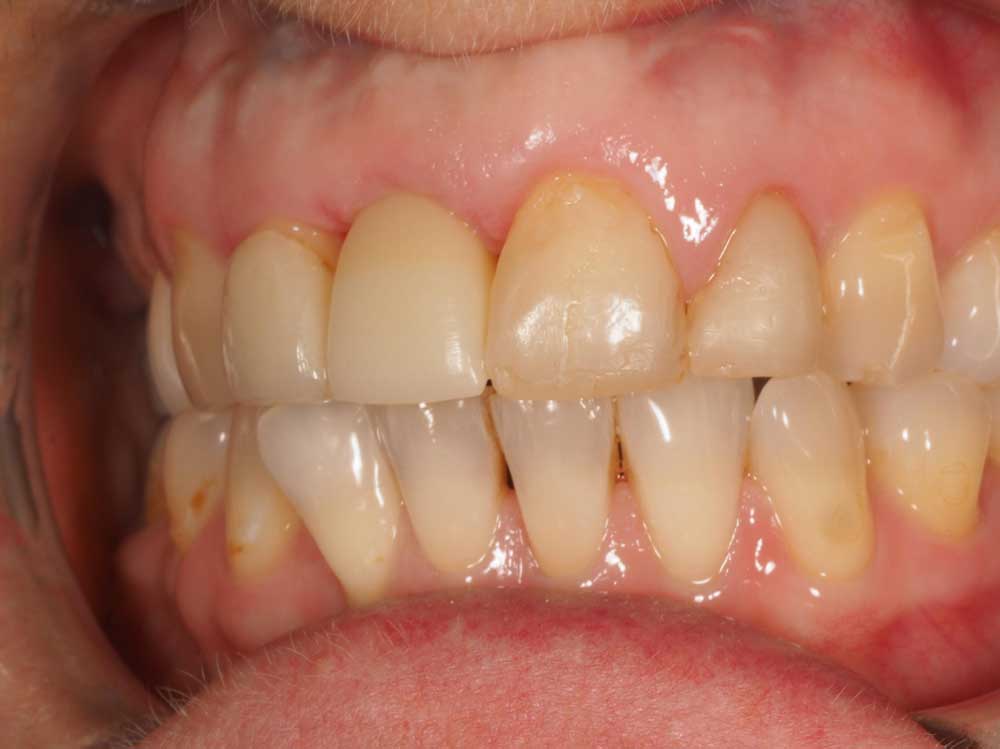
Fig 2 – shows a different perspective, with composite and old veneer work clearly visible.
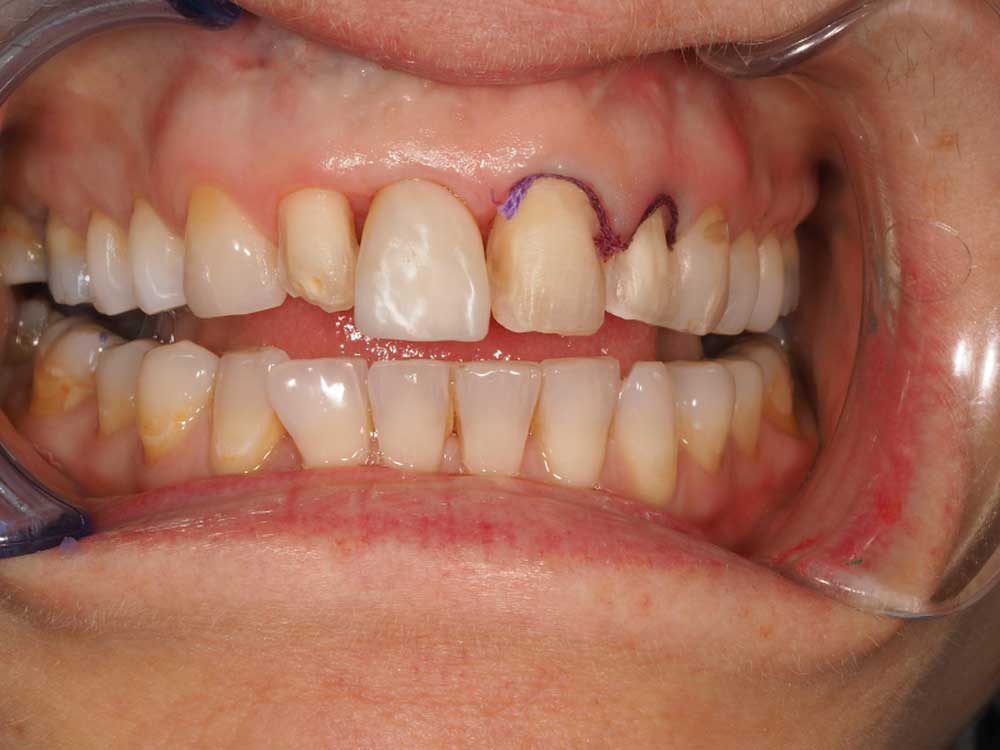
Fig 3 – shows veneer preparations and loss of interproximal papilla.
THE Process
During our consultation, Kathy was hugely reluctant to smile, and even when asked for her biggest smile for photographs it was more of a grimace. It was very apparent that we could, of course, improve on what we were presented with but it was also very apparent that our lovely patient had invariably become very dentally aware. Looking at the smallest of details, from tiny blemishes in her current restorations to discrepancies in subtle line angles, on the whole, a very tricky situation and one with which to tread very carefully.
Patients like Kathy must be treated and managed gently and slowly, and in a strange way without involving them too much at this stage with huge amounts of decision-making.
This in part comes down to the fact that a patient has already decided that you are the best team to help them so bombarding them with “Well do you like this or do you like that” often leaves them feeling a little unsure. And in severe cases can result in the loss of complete confidence.
Now with the loss of Kathy’s UL1, it has meant that there has unfortunately been significant tissue loss creating large triangles with which to fill. Added to that we will now be restoring teeth 11, 12, and 21 with veneers, replacing old restorations and old composite work, with minimally prepared teeth with all but one having margin lines supra-gingival has meant that closing these dreaded triangles will be almost impossible. We will now be totally reliant on the soft tissue contouring of the implant restoration pushing the papilla into these undesirable spaces without applying much pressure.
Aside from these biological issues, we will have to overcome the fact that the veneers will be fabricated in Emax (Lithium Disilicate) and the implant restoration using a Ti-Base solution will be constructed from Zirconia, as vital as this choice of restoration can be the way in which it will behave in varying lights, least of all the fact that there will be a silver Ti-Base shining through the reflective properties of the inner core can present many issues when matching to natural teeth let alone matching them to veneers with varying levels of vitality in the standing teeth.
I didn’t feel shape would be an issue especially given we would have little choice but to go for a more rectangular tooth form with the need to close those triangles.
A rectangular tooth form would allow for us to work with shallow line angles closing spaces and yet avoiding unwanted shadows that can be experienced in restorations being too bulky with say a rounder form, especially with such minimal preparations and the shallow emergence being caused by a supra-gingival finish line.
I think it is important to give an honest representation in the view that the reader can gain more from it even if it is from the “Oh, I’ve been there” a point of view.
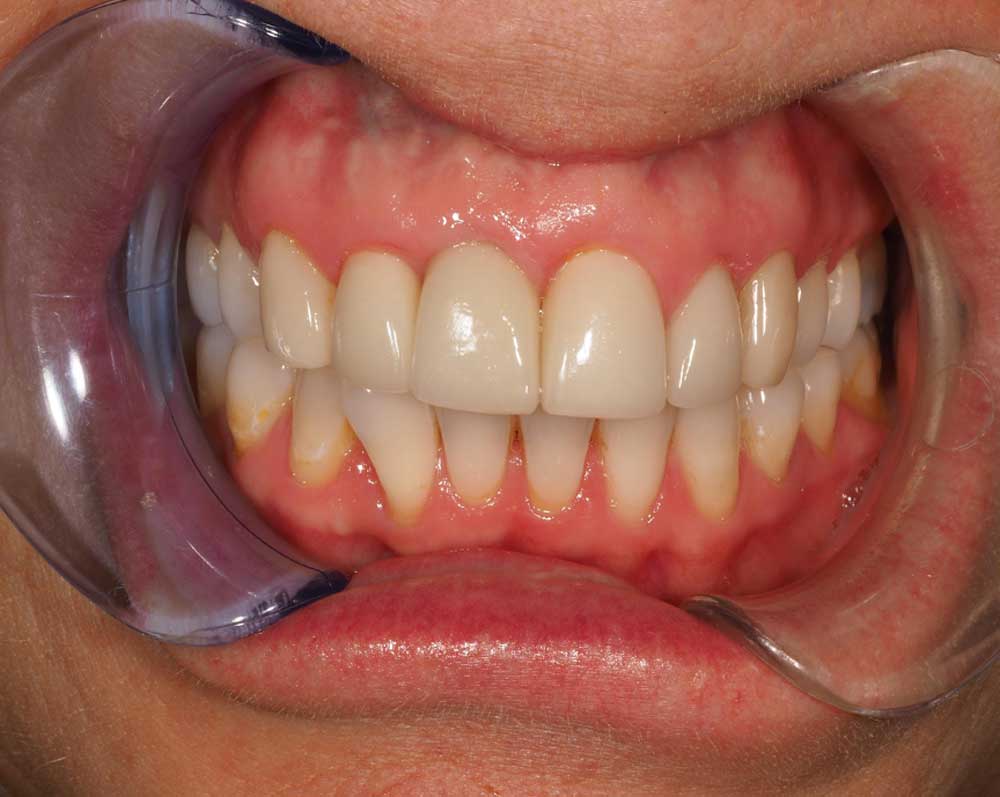
Fig 4 – Shows the disparity at one of the first attempts with the Ti-Base shining through the implant restoration on UR1, but it is important to mention that through good dialogue with the patient there was a greater understanding that A: we were heading in the right direction and B: it didn’t need the patient to high light we could do better, that in itself will the patient the reassurance that the journey is nearing completion, as a result, you will always end up with a much happier patient.
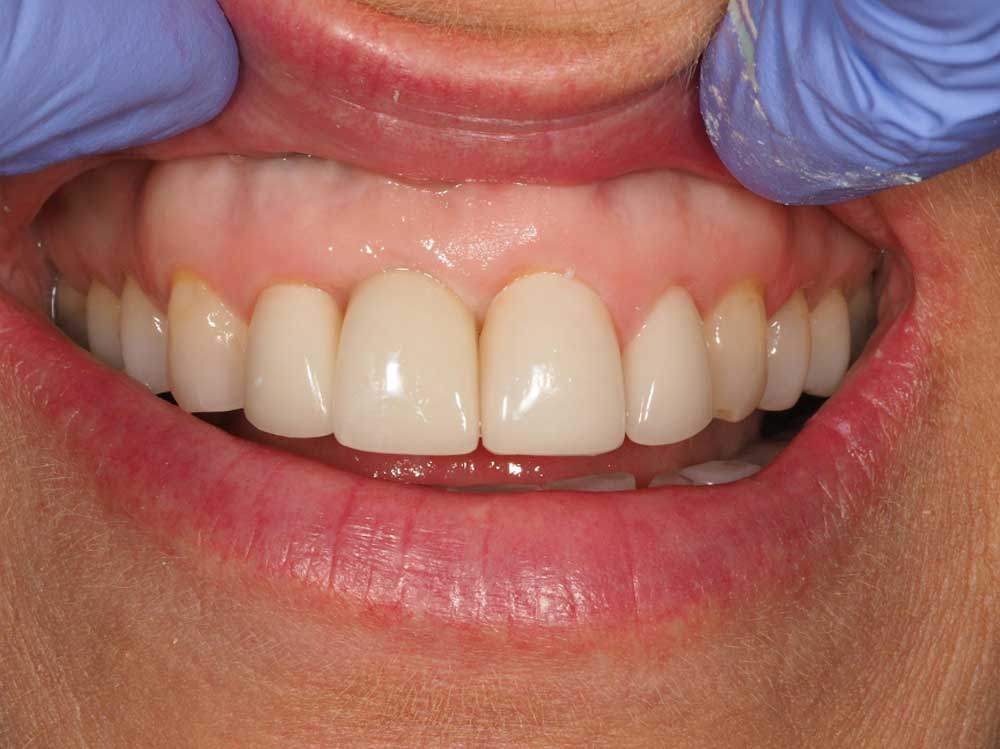
Fig 5 – Shows the restorations at fit, and although the differences were subtle in the final result, I believe the overall appearance is far more harmonious, with softer embrasures and the reduction in translucency in part aided by using MO pellets as oppose to LT for the Emax veneers and MO substructure for the Zirconia implant restoration, all that was required to complete the tooth forms was some minimal veneering, limited to just incisal powders.
THE RESULTS
Now, this case actually took three attempts. The first two attempts being a result of aesthetic issues trying to match the veneers with an implant restoration, and the third attempt coming by way of the changes that the patient wanted to implement as she traveled through her journey.
What we had learned through the first two attempts was that we would have to deliberately kill off too much translucency to help us restore the implant crown more easily. Simplicity is key.
Of course, there is the argument of “So why didn’t you make the crown from Emax in the first place instead of Zirconia”? Well, there are a number of issues with that.
Firstly, and most importantly, we are in the fortunate position to be based in a referral practice, this gives us a huge insight as to what is working and what isn’t.
Over the years we have seen a large number of Emax crowns that have failed when they have been used with Ti-Base solutions.
Of course, adaptations can now be implemented with the use of Atlantis GoldHue™ abutments, but our protocol at the time and still is, for all but a few cases, to work with standard Ankylos Ti-Base. In our view this simplifies the process for both the patient and the referring practice, should anything need addressing in the future.
Case study by Tony Atkins, Senior Technician
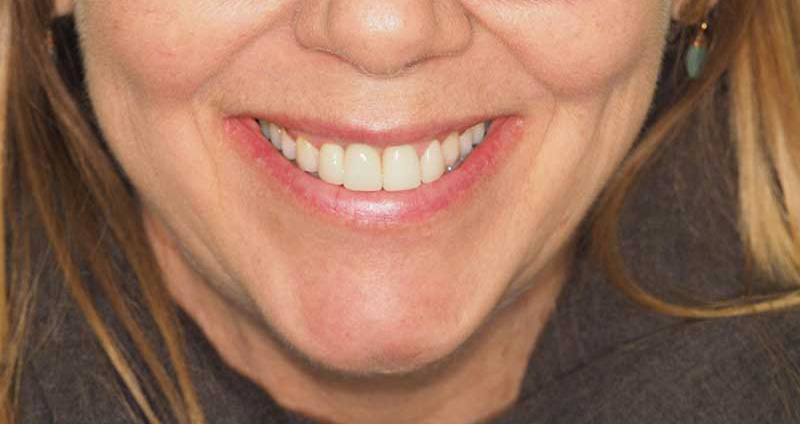
And a patient who once couldn’t smile at all now unable to stop smiling!
Ultimately it is the patient who will indicate whether or not the case is a success.
Allowing the patient the time they need to express their likes and dislikes without feeling like they are being unreasonable, will ultimately see a result that everyone will be very proud of.
Let's work together

